[ad_1]
The tip of the Medicaid steady enrollment provision in March 2023 and the resumption of Medicaid disenrollments after a three-year pause all the way through the pandemic are more likely to refocus consideration on gaps in Medicaid protection within the ten states that experience now not followed the Inexpensive Care Act’s (ACA) Medicaid growth as of March 2023. Throughout the pandemic, Medicaid enrollment larger and the uninsured price dropped in large part because of steady enrollment. As soon as Medicaid disenrollments resume, the collection of people who find themselves uninsured is anticipated to extend and may just upward push extra steeply in non-expansion states. In growth states, as a result of all adults with earning as much as 138% of the federal poverty stage (FPL) are eligible for Medicaid, many present enrollees will stay eligible even supposing their earning have risen. Then again, in non-expansion states, with eligibility thresholds steadily slightly low and in large part restricted to oldsters, lots of the ones with earning beneath poverty who’re now not eligible for Medicaid is not going to have get admission to to an reasonably priced protection choice and can most probably change into uninsured.
Particularly, two states have taken contemporary motion to undertake the Medicaid growth. In November 2022, electorate in South Dakota authorized Medicaid growth via a poll measure and in March 2023, regulation adopting the Medicaid growth in North Carolina was once signed into regulation, despite the fact that growth is contingent on passage of a state price range later within the 12 months. If growth proceeds as anticipated in North Carolina, it’ll change into the 41st growth state (together with the District of Columbia), leaving ten states that experience now not followed the growth. This temporary gifts estimates of the quantity and traits of uninsured folks within the ten non-expansion states who might be reached via Medicaid if their states followed the Medicaid growth the usage of information from 2021, the latest 12 months to be had. It will have to be famous that this research makes a speciality of the collection of uninsured individuals who can be newly eligible if non-expansion states followed the growth; the whole quantity of people that would change into eligible for Medicaid is bigger as it contains folks with earning 100%-138% FPL who’re recently enrolled in Market protection in addition to some who could have different protection. An summary of the technique underlying the research can also be discovered within the Data and Methods, and extra element is to be had within the Technical Appendices.
What’s the protection hole?
The protection hole exists in states that experience now not followed the ACA Medicaid growth for adults who aren’t eligible for Medicaid protection or subsidies within the Market. The ACA expanded Medicaid to nonelderly adults with revenue as much as 138% FPL ($14,580 every year for a person in 2023) with enhanced federal matching price range (now at 90%). This expanded eligibility for low-income folks and newly established Medicaid protection for adults with out dependent youngsters; on the other hand, the growth is successfully not obligatory for states on account of a 2012 Perfect Courtroom ruling. As of March 2023, 41 states together with DC have expanded Medicaid (Determine 1). As famous above, North Carolina has followed the Medicaid growth contingent on passage of a state price range later this spring.
In the rest ten states that experience now not followed the Medicaid growth an estimated 1.9 million folks fall into the protection hole. Adults who fall into the protection hole have earning above their state’s eligibility for Medicaid however beneath poverty, making them ineligible for subsidies within the ACA Marketplaces (Determine 2). When enacted, the ACA didn’t look ahead to that states can be accepted to forgo Medicaid growth; as such, subsidies within the Marketplaces aren’t to be had for folks with earning beneath poverty.
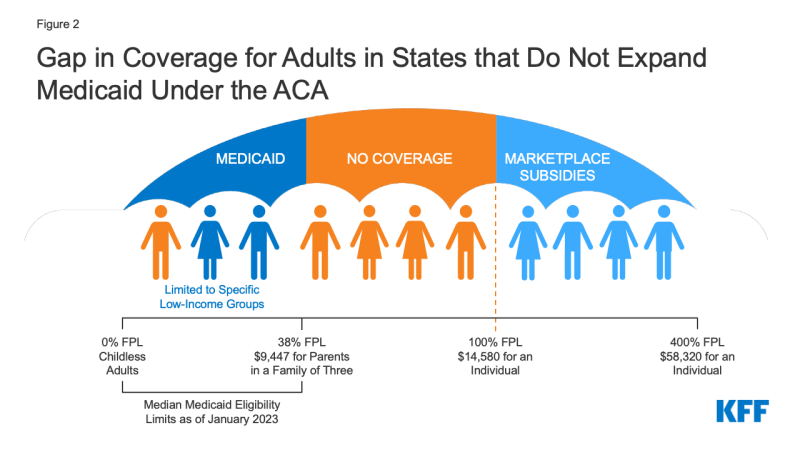
Determine 2: Hole in Protection for Adults in States that Do No longer Amplify Medicaid Below the ACA
Medicaid eligibility for adults in states that experience now not expanded their techniques could be very low. In those states, the median revenue prohibit for fogeys is solely 38% FPL, or an annual revenue of $9,447 for a circle of relatives of 3 in 2023, and in just about all states now not increasing (apart from Wisconsin via a waiver), childless adults stay ineligible without reference to their revenue (Determine 3). In Texas, the state with the bottom eligibility threshold, folks in a circle of relatives of 3 with earning above $3,977 every year, or simply $331 per 30 days, aren’t eligible for Medicaid. As a result of there is not any pathway for protection for childless adults, apart from in Wisconsin, greater than three-quarters (76%) of folks within the protection hole fall into this crew.
States that experience now not carried out the growth have uninsured rates which are just about double the speed of growth states (15.4% in comparison to 8.1%). Folks with out insurance policy have worse get admission to to care than people who find themselves insured. One in 5 uninsured adults in 2021 went with out wanted hospital treatment because of charge and uninsured persons are much less most probably than the ones with insurance coverage to obtain preventive care and services and products for main well being stipulations and protracted illnesses.
What are the traits of folks within the protection hole?
Adults left within the protection hole are concentrated in 3 states within the South. 4 in ten folks within the protection hole are living in Texas, which has very restricted Medicaid eligibility, and because of this, a big uninsured inhabitants (Determine 4). One in 5 folks within the protection hole reside in Florida, and 13% in Georgia. In overall, 97% of the ones within the protection hole reside within the South. Seven of the 16 states within the South have now not followed the Medicaid growth, and the area has extra deficient, uninsured adults and higher uninsured rates in comparison to different areas.
Folks within the protection hole are disproportionately folks of colour. Nationally, over six in ten (61%) folks within the protection hole are folks of colour, a proportion this is upper than for non-elderly adults in most cases in non-expansion states (47%) and for non-elderly adults national (40%) (Determine 5). Those variations partly give an explanation for persisting disparities in health insurance coverage by race/ethnicity.
Regardless of having low revenue, just about six in ten folks within the protection hole are in a circle of relatives with a employee, and just about part are running themselves (Determine 6). Adults who paintings would possibly nonetheless have earning beneath poverty as a result of they paintings low-wage jobs. Folks with earning beneath poverty steadily shouldn’t have get admission to to employer based totally medical insurance or if to be had, it’s steadily unaffordable. The commonest jobs amongst adults within the protection hole are cashier, cook dinner, waiter/waitress, building laborer, maid/housecleaner, retail salesclerk, and janitor. For fogeys in non-expansion states, even part-time paintings would possibly cause them to ineligible for Medicaid.
Some folks within the protection hole have important present well being care wishes. KFF research of the 2021 American Group Survey presentations that a couple of in six (15%) folks within the protection hole have a practical incapacity, that means they have got critical problem with listening to, imaginative and prescient, cognitive functioning, mobility, self-care, or impartial residing. Even with practical disabilities, many aren’t in a position to qualify for Medicaid via a incapacity pathway leaving them uninsured. Older adults, age 55-64, an age of accelerating well being wishes, make up 17% of folks within the protection hole. Research has demonstrated that uninsured folks on this age vary would possibly go away well being wishes untreated till they change into eligible for Medicare at age 65.
What number of uninsured may just acquire protection if all states followed the growth?
If all states followed the Medicaid growth, roughly 3.5 million uninsured adults would change into newly eligible for Medicaid. This quantity contains the 1.9 million adults within the protection hole and an extra 1.6 million uninsured adults with earning between 100% and 138% FPL, maximum of whom are recently eligible for Market protection however now not enrolled (Determine 7 and Desk 1). Lots of the adults who’re recently eligible for protection within the Market qualify for plans with zero premiums; on the other hand, even without a premiums, Medicaid may provide extra complete advantages and decrease cost-sharing in comparison to Market protection. The possible quantity of people that might be reached via Medicaid growth varies via state.
Whilst now not counted within the numbers above, there are an estimated 173,000 folks within the protection hole and 154,000 uninsured adults with earning 100%-138% FPL who will change into eligible for Medicaid if Medicaid growth proceeds in North Carolina with the passage of the cheap (Desk 2). There are an extra 281,000 folks in North Carolina who’re recently insured within the ACA market with earning 100%-138% of FPL who will change into newly eligible for Medicaid with growth.
What’s the outlook forward?
Virtually ten years after implementation of the Medicaid growth in January 2014, a considerable frame of study issues to in large part sure results. KFF reviews printed in 2020 and 2021 reviewed greater than 600 research and concluded that growth is connected to features in protection, development in get admission to and well being, and financial advantages for states and suppliers. Extra recent studies in most cases in finding sure results associated with extra explicit results akin to progressed get admission to to care, remedy and results for most cancers, persistent stipulations, sexual and reproductive well being and behavioral well being. Research additionally level to proof of diminished racial disparities in protection and get admission to, diminished mortality and enhancements in financial impacts for providers (specifically rural hospitals) and financial steadiness for people.
Whilst makes an attempt to go federal regulation to handle the protection hole nationally failed, states that newly put in force Medicaid growth will obtain a temporary fiscal incentive underneath the American Rescue Plan Act (ARPA). Below ARPA, states that newly undertake growth are eligible for an extra 5 share level building up within the state’s conventional fit price (FMAP) for 2 years. This incentive does now not observe to the growth inhabitants; states are required to hide 10% of the price of Medicaid growth, with the government overlaying 90%.The standard FMAP applies to maximum spending for all non-expansion teams (youngsters, folks and folks eligible in keeping with age 65 plus or incapacity); Medicaid spending for non-expansion teams is way greater than spending for the growth crew. KFF analysis presentations that each one non-expansion states may just see a web fiscal get advantages over a two-year duration in the event that they followed the growth. For the 2 states that lately followed the growth, South Dakota and North Carolina, the estimated fiscal get advantages is $60 million and $1.2 billion, respectively.
Seven of the remaining 8 states to undertake growth did so via a poll measure; on the other hand, that’s not an choice in maximum different non-expansion states. Each and every state, apart from North Carolina, that has adopted growth since 2019 has carried out so now not via legislative or govt processes, however on account of a a hit poll initiative. Maximum lately, in South Dakota electorate authorized a poll query in November 2022. Even though growth poll projects had been a hit in all seven states the place they have got long past to electorate (Idaho, Maine, Missouri, Nebraska, Oklahoma, and Utah), lots of the final non-expansion states shouldn’t have ballot initiative processes. North Carolina is the primary state to undertake growth via a legislative procedure since Virginia followed in 2019.
Enlargement may just lend a hand stem will increase within the collection of people who find themselves uninsured because the Medicaid steady enrollment provision ends and states resume disenrollments after a 3 12 months pause all the way through the pandemic. All states have skilled important Medicaid enrollment growth on account of regulation enacted early within the pandemic that prohibited states from disenrolling folks from Medicaid in trade for enhanced federal matching price range. The rise in Medicaid protection has been a key issue contributing to the decline in the uninsured price. When the continual enrollment provision expires on March 31, 2023 and states resume common Medicaid disenrollments, tens of millions are anticipated to lose Medicaid if they’re now not eligible or in the event that they face limitations finishing their renewals. Whilst most of the people who’re decided to now not be eligible in growth states will qualify for different protection, both throughout the Market or via an employer, in non-expansion states, deficient folks who’re now not eligible for Medicaid will most probably fall into the protection hole and change into uninsured.
[ad_2]
Source link


